Otolaryngology:
Nose Conditions
When you have a blocked tear duct, or a nasolacrimal duct obstruction, your tears can't drain normally, leaving you with a watery, irritated eye. Blocked tear ducts are caused by a partial or complete obstruction in the tear drainage system. This condition is almost always is correctable. Treatment depends on the cause of the blockage and your age.
Failure of the thin tissue at the end of the tear duct to open normally is the most common cause. In adults, a blocked tear duct may be due to an injury, infection or a tumor. (Blocked tear ducts are very common in newborns, but they usually get better without any treatment during the first year of life.)
Blocked tear ducts can happen at any age.
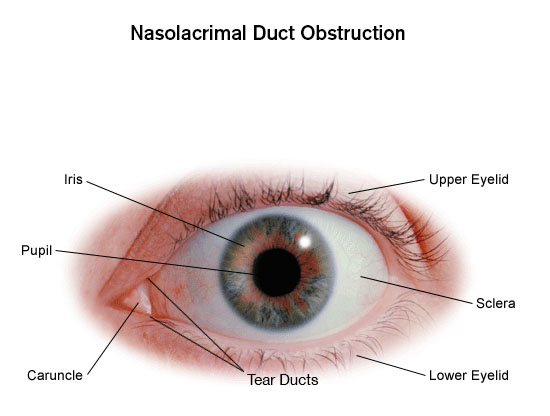
Symptoms of nasolacrimal duct obstruction often affect only one eye and include:
You should consult with an otolaryngologist if your eye is constantly watery and continually irritated or infected. In rare cases, blocked tear ducts are caused by tumors pressing on the tear drainage system for which immediate treatment is necessary.
Tests to diagnose a blocked tear duct include:
Your otolaryngologist will work with you to determine which treatment is right for your specific condition.
You will receive a thorough diagnostic examination to evaluate if you have a nasolacrimal duct obstruction and determine what course of treatment is needed. Careful monitoring and the involvement of an experienced otolaryngologist are important to the successful outcome for patients with ear, nose and throat disorders and conditions.
If you are having surgery or a procedure, you will likely be scheduled for a visit to the Weiner Center for Preoperative Evaluation for pre-operative information and tests.
The day of surgery, you will be taken care of in the operating room by otolaryngologist, anesthesiologists and nurses who specialize in surgery for patients with nasolacrimal duct obstructions. After surgery, you will go to the post-surgical care unit where you will receive comprehensive care by experienced surgical and nursing staff.
Brigham and Women’s Faulkner Hospital provides a multidisciplinary approach to patient care by collaborating with colleagues who have extensive experience in diagnosing and treating ear, nose and throat disorders and conditions. In addition, patients have full access to Brigham and Women's Hospital's world-renowned academic medical community and state-of-the-art facilities.
Offering comprehensive medical, surgical and psychiatric care as well as complete emergency, ambulatory and diagnostic services to residents of southwest Boston and the surrounding suburbs.
Learn more about BWFH