According to the Centers for Disease Control and Prevention, one in three patients who die in the hospital has sepsis, which is a medical emergency caused by the body’s extreme response to an infection. Sepsis occurs when an infection, such as pneumonia, causes an overwhelming response by the immune system resulting in organ dysfunction. The most common symptoms of sepsis are low blood pressure, elevated respiratory rate, altered mental status, shock index greater than 1 (in which the HR is >SBP), decreased urine output, elevated creatinine, elevated bilirubin and decreased platelet count. Patients who look acutely ill, have a possible infection, have risk factors such as being older than 65 and have other comorbidities most likely have sepsis.
“At Brigham and Women’s Faulkner Hospital, the Sepsis Workgroup tracks two sets of quality measures related to sepsis—the Mass General Brigham Internal Performance Framework (IPF) and the Centers for Medicare & Medicaid Services (CMS) SEP-1 measure, which is publicly reported in order to continuously improve the quality of our sepsis care,” says Katy O’Loughlin, MPH, Quality Improvement Analyst at BWFH. “Both measures include several time-based elements with best practices for sepsis care.”
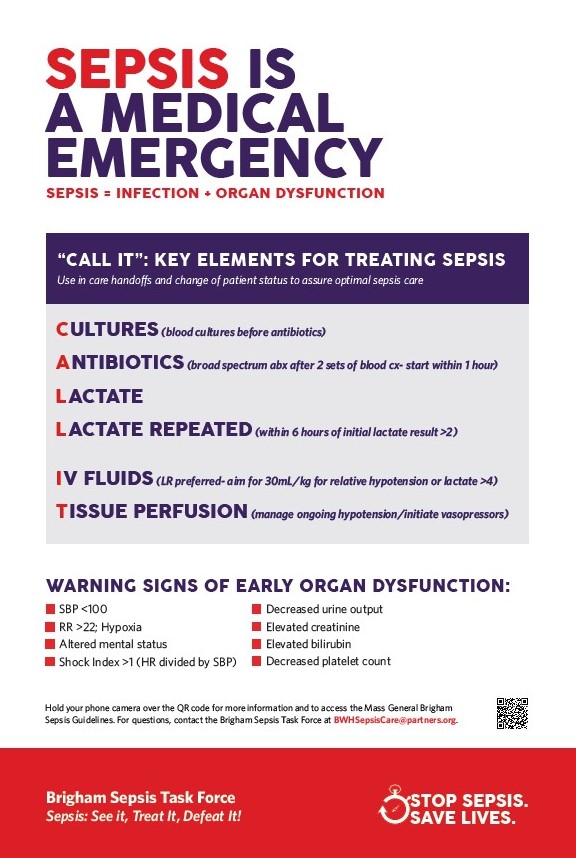
To remember those best practices, simply CALL-IT:
“At BWFH we want everyone to CALL-IT if your patient meets the criteria—it could save their life!” stresses Beth Waters, MSN, RN, CPEN, Nursing Professional Development Manager for the Emergency Department, Nursing Supervisors and PCA Float Pool.
According to O’Loughlin, BWFH’s Sepsis Workgroup has been successful in increasing performance related to the timing of the blood culture draw through an improvement effort led by the Emergency Department and the Lab where stickers are used on blood cultures to indicate a blood draw of a septic patient. “The ED nurse writes the time of draw on a sticker, allowing the Lab technician to record the proper collection time so that Epic documentation accurately indicates a draw before antibiotics are administered,” explains O’Loughlin. “Pre-implementation, blood culture element performance was 77.6 percent. Since April of 2020 when this project was rolled out, performance has increased to 88.4 percent—that’s more than a 10 percent improvement.”
The BWFH Sepsis Workgroup has also recently expanded. They now meet monthly and include the Nursing Professional Development Managers, Pharmacy, Nursing Informatics, the Lab, and nurse and physician representation from the ED, med/surg and the ICU. They recently collaborated to create a new smart phrase available to providers in Epic that helps meet the CMS documentation requirements that are necessary when a provider administers less than the CMS measure required 30mL/kg of crystalloid fluids because of concerns related to a patient’s history of congestive heart failure or renal disease.
Currently, the BWFH Sepsis Workgroup is seeking to improve BWFH’s performance with the CMS SEP-1 measure by addressing failures related to the fluids perfusion element. For the Mass General Brigham IPF measure, they are working to meet the goal of 71 percent performance by the end of 2021.
If you are interested in sepsis care and/or have ideas on how to improve sepsis performance in your unit, we welcome you to join the BWFH Sepsis Workgroup! Additionally, if you have any questions about the information shared here or either of the sepsis quality measures, please reach out to Katy O’Loughlin at kcoloughlin@bwh.harvard.edu.
Looking for more news from BWFH? Go to News to find articles about health, updates to our programs and services and stories about staff and patients.
Go to News